It’s all about the details. Pick your thumbnail image, add closed captions, update settings, and track your video performance analytics in the video library. Manage video settings. Learn more about the video library.
Notes On The Testing Methods Discussed
Prick or scratch tests and hyposensitization
The mainstay of conventional allergy test has not advanced significantly since 1911, when the prick and scratch test method was first developed. For this method a small drop of the substance being tested is dropped onto the skin, which is then scratched or pricked with a needle at that spot. The amount of flare and wheal compared to that caused by a control (inert) solution gives an indication of how allergenic the substance is (Noon L., Prophylactic Innoculation against Hay Fever, Lancet 1, London, 1911, p. 1572).
It is a very inaccurate method, with many false negatives, and subjects seldom react to food at all in this way, though a demonstrable allergy may be present on challenge testing. An important migraine study at the Great Ormond Street Hospital for Sick Children in 1983 showed that none of the cases would have recovered by following an exclusion diet based on the results of the prick testing included in the trial, though 93 per cent improved on a suitable diet, showing that food allergy was the cause (Egger J. et al. Is Migraine Food Allergy? Lancet, London, 15 Oct 1983, pp.865-8).
False negatives: are disastrous because you are misled into believing the substance is safe
False positives: are merely inconvenient, you avoid something unnecessarily, when it is quite safe
One final failure, which is not talked about: the substance with the largest reaction may NOT be the one which is causing you the most trouble, as I have found out many times with the help of Miller’s Method.
The hyposensitization method aims to find out which substances the patient is allergic to, by giving a whole batch of prick testing, and then to administer injections of a mixture of these, increasing gradually in strength, until quite large amounts are being tolerated. The body is often then found to be able to cope with normal ambient concentrations.
There are two major drawbacks to this hyposensitization treatment:
- it rarely works for food and
- it can be extremely dangerous. Patients sometimes react severely and deaths due to anaphylaxis occured regularly until by common consent its use was abandoned in 1986, except in special circumstances and where full cardio-pulmonary resuscitation equipment is at hand.
The only suitable indications for the use of this method are in cases of perennial rhinitis and asthma due to dust and dust mite allergy, seasonal rhinitis due to pollens and the danger of anaphylaxis due to insect stings. Even so, very brittle (vulnerable) cases, especially children, are better left un-desensitized, since the dangers of the method are very real.
Patch testing
Another fairly primitive technique is patch testing. Small quantities of different suspected substances are placed under individual cups which are taped to the skin for a number of hours. A reddening of the skin under the patch denotes a sensitivity to that substance. A control is used, since some people react to the pads or tape, etc.
A positive reaction is probably fairy dependable, but it rarely happens. Unfortunately, even substances known to have a marked effect often don’t affect the skin. In other words, negative reactions do not exclude significant allergens.
This method works best for identifying causes of contact dermatitis, such as nickel, soap powders or industrial chemicals.
Immunological tests
All other conventional allergy tests are based on immunological reactions of the IgE antibody type. Naturally, classic antigen-antibody reactions are the only results to be expected, which precludes a large number of other allergic and intolerant reactions.
Broadly speaking, then these tests are fine if they give a positive result; which is to say, if an allergy to wheat or egg is found, it exists. Avoiding that food will help with the overall body load. But negatives are meaningless (these occur over 95 per cent of the time). Also, a positive reaction on an immunological test only means antibodies are present, it does not mean the allergy is the one causing symptoms. Experts often overlook this elementary point.
The RAST (radio-allergo sorbent) Test
This is the basic immunological test using labeled molecules for quantifying results.
Specific antigen (in this case the allergy being tested) is incubated in contact with a plastic plate or tube until it becomes bound by adsorption (adhesion).
The plate is washed and the patient’s serum, with suspected IgE antibody to that allergy, is added. This naturally locks on to the antigen. Unused sample fluid is washed away, leaving “captured” IgE.
How much IgE antibody has been ‘captured’ is measured by adding a second binding antigen, in this case anti-IgE, which locks onto the IgE in the antigen-antibody complex. This creates an antigen-IgE-antigen “sandwich”.
After all un-fixed substances have been washed away, the amount of IgE antibody that remains sandwiched can be measured by a number of tricks. In the basic test, the anti-IgE is labeled with radio active iodine125. After unused labeled molecules have been washed away, the amount that remains behind can be measured using a gamma counter (Geiger counter). Hence: radio-allergo sorbent test.
Another variation called the ELISA test (enzyme-labelled immuno sorbent assay) is to label the anti-IgE with a colour-generating chemical (enzyme). After washing, adding a second enzyme releases the dye. Sensitive spectrometry measures how much colour is now present, hence giving an indication of how much IgE is present.
This approach gives an exquisitely sensitive measurement of how much antibody was present in the serum being tested, using only tiny amounts of test solutions. If the RAST or ELISA test are positive, then antibody is present and a degree of allergy exists to that substance. Very large amounts of IgE mean a bad allergy and a potentially dangerous reaction.
Provocation Tests
Conventional allergists share with clinical ecologists a respect for using the patient as his or her own test bed. To administer a substance to the patient to see what happens is called a provocation test. Food and chemical challenge tests are described elsewhere in this section, since they are not used by conventional allergists.
Ophthalmic Testing: Small quantities of test reagent can be placed into the conjunctival sac of the eye. Reactions include visible reddening, lachrymation (tears) and (sometimes) sneezing. There is a limit to the number of substances that can be tested at any one time (i.e., very few) and so this has limited application. It is particularly suitable for seasonal reactions (pollens) being tested out of season.
Nasal Provocation Challenge: Potential allergens can be introduced into the nasal passages, either as liquid or powder particles, and the results monitored. The patient is then observed for an arbitrary 5 to 30 minutes (depending on the standard procedure). Reactions can include sneezing, catarrh, a blocked nose and, naturally a clinical ecologist would ask, cerebral and other manifestations as well. One or two initial sneezes are discounted as being probably just a normal response to the irritating effect of the liquid/powder in the nasal passages.
Alternate nostrils are used and up to 20 items can be tested in one session. If severe symptoms develop, a nasal ‘washout’ using saline (salt water) will normally clear them. It not, testing may have to be discontinued for the day.
Bronchial challenge test: The patient is asked to inhale the test substance into their lungs. It is very dangerous indeed, people have died. No responsible physician should ever administer such a test, yet conventional allergists sometimes do. If you are offered it, refuse outright. Two deaths I know of were attributable to research testing, using this method; the unfortunate patients believed they were helping science.
NON-CONVENTIONAL ALLERGY TESTING METHODS
These can generally be classified as the good, the bad and the downright awful. Remember that the value in the test method may lie as much in the treatment which goes with it as the actual technique itself. For that reason I introduce first an entirely scientifically credible testing option which gives good accuracy and leads to a treatment method that has spelled freedom and health for countless patients. I myself have taken over 10,000 people through it over the decades since I was shown it. Conventional allergists fight it tooth and nail, entirely through vested interest. The controversy rages on. You are provided with some references to clinical trials, which you may pursue for yourself.
Miller’s Method (provocation-neutralization)
Also known as serial end-point skin titration, this is the method that enabled me to find some remarkable and obscure allergies, which would otherwise probably have remained hidden.
It was first developed by Carleton Lee of Missouri in the late 1950s. Lee began a series of investigations by injecting his allergy patients with antigens at different concentrations. He noticed something interesting: obviously sometimes he provoked a symptom but sometimes, given a particular dilution, a patient’s symptoms would disappear in just a few minutes, as if by magic. This might happen, eben if the patient had arrived at the office with symptoms! It was one of those lucky situations where the right person is in place, at the right time, to draw useful scientific conclusions. Lee realized immediately that diluting an antigen could make it effective at neutralizing the symptom associated with the allergy.
In fact it emerged that only one specific dilution had this serendipitous effect, which Lee christened the “neutralizing dose”; unfortunately, it was different for each patient (and each allergen) and had to be tested individually. But it was a major advance and offered much symptomatic relief for suffering patients. Herbert Rinkel and others went on to improve Lee’s method and promote its more widespread use, and the first definitive book explaining the technique in detail was written by Joseph B. Miller (Food Allergy: Provocative Testing and Injection Therapy, Charles C. Thomas, Springfield, Illinois, 1972); hence known as Miller’s method.
Lee’s widow has (quite rightly) campaigned to have it recognized as the Lee-Miller method. I should also say at this point that Joe Miller is a nice unassuming man and would not dream of purloining a colleague’s eponymous title but that’s the way of the world.
The technique
After testing the control and being assured of the zero baseline reaction, a reagent (food, dust or chemical) is injected superficially into the skin (intracutaneously), making a deliberate wheal. If this grows compared to the control over, say, 10 minutes, this suggests an allergy. The bigger the wheal, the more probable the culprit up to a point. Thus far it looks like scratch or prick testing; but because of the safety factor implicit in the explanation below, we use quite concentrated reagents, which cause foods to show up often, unlike with the scratch or prick method.
Here’s a shot of my nurse Sue administering the testing in a friendly/informal lab setting:

Sometimes a symptom is produced (provocation) and this is much more conclusive. Remember these substances are tested one at a time, so there is usually no doubt which caused the symptom.
If a reaction occurs (wheal or symptom), the patient is then given a series of weaker and weaker injections of the same substance at 10-minute intervals until the wheal ceases to grow and the symptom, if there is one, disappears completely.
This ‘switch-off’ dilution is called the neutralizing dose; it works as a kind of antidote. The procedure is illustrated in the figure below.
Safety note: Because of the ultimate neutralization of the allergic reaction, this method is very safe. Even very unpleasant symptoms are brought rapidly under control by injecting a more dilute dose of the allergen (nearer the end-point). Final adjustment of the correct end-point means that symptoms have vanished altogether. In over half a million test doses I only ever once encountered anaphylaxis, which was blocked by immediate administration of epinephrine (adrenalin). At the time of writing no death has occurred due to Miller’s method, despite its use by thousands of doctors world wide. This is in sharp contrast to the hypo-sensitization method, which caused multiple deaths annually until discontinued.
Nevertheless it is sensible to avoid injecting any substance into a patient who has already had an anaphylactic reaction.
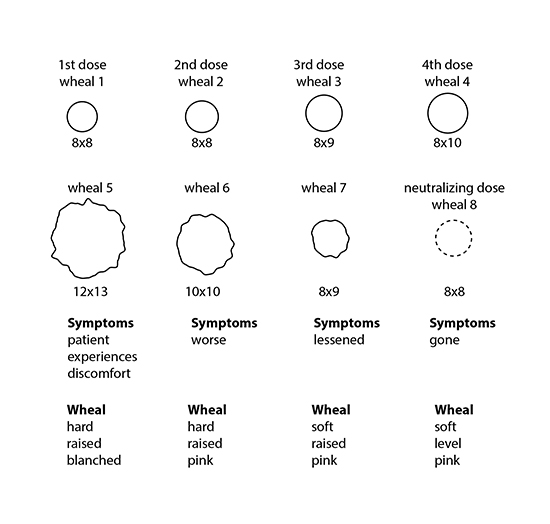
The size of the wheal at start is unimportant
After testing a number of substances, a patient can then be given a cocktail of the resulting neutralizing doses. These are administered by self-injection every second day (a simple procedure, easily learned). Some clinics allow patients to take the neutralizing complex sublingually. This has the appeal of being easier and without any discomfort but gives less efficient cover. Sublingual administrations are needed every few hours (just prior to each main meal), which can be a nuisance. The beauty of neutralization is that patients can (usually) go ahead and eat the allergy food. Obviously common sense must play a part and if the reaction is severe, reduced intake may be necessary. But it is better than a life of strict avoidance. Happy patients have found themselves able to eat and drink troublesome items and so rejoin social life on virtually equal terms with the rest of us.
Coordination testing
The method’s accuracy can be increased by asking the patient to undertake simple tasks, such as a handwriting demonstration and noting how these change under testing. At the neutralization point the patient’s performance should return to normal. More objective determinations can include measuring the patient’s pulse rate and blood-pressure.
One important advantage to this method is that the symptom provoked gives the patient a vivid subjective demonstration of each allergen, which helps to fix it in his or her mind. This is far more meaningful than the abstract results of a blood test or some other laboratory report. But remember, not all allergens provoke symptoms.
Another advantage is that a patient with multiple allergies need not be restricted to a very meager diet: allergenic foods can be eaten in moderation, under the umbrella of the ‘drops’. Only foods that cause a severe reaction are banned – and the patient may even become desensitized to these by taking the drops and avoiding the food for several months.
Problems
When it works, the method works very well. A number of difficulties may occur, however. About 10 per cent of cases are plagued with shifting end-points. Repeat testing becomes necessary and this is troublesome and may be expensive. These shifts can occur very rapidly. So that by the time the patient is supplied with his or her prescription, it is ineffective. In these cases, even retesting won’t help. However, this only applies to less than 5 per cent of those tested.
Unfortunately, the people who need this kind of treatment most, the very sick, ‘unstable’ patients, are the ones most likely to be troubled by this shifting end-point phenomenon.
Even if the antidotes are not effective, however, the method is still good for diagnosis. It can pinpoint rapidly the worst allergens for a patient. This will help reduce his or her body load. The method is also very safe. Reactions are common but rarely severe, and in any event can be relieved rapidly by the corresponding neutralizing dose. Nevertheless, it would seem prudent to avoid injecting anything into an individual who has experienced a dangerous anaphylactic reaction.
An outstanding feature of this neutralizing technique is that it is usually effective against environmental chemical triggers – no other method is. This makes it superior in my view to enzyme potentiated desensitization.
Hormones
An important special application of Miller’s method is in neutralizing hormones. Women tested with oestrogens and progesterone often experience reactions, particularly to progesterone in cases where the woman deteriorates badly health-wise at around her period time. We can hypothesize that these women are allergic to their own hormones (see hormones and allergy).
In fact there are two phenomena we encounter. If the reaction is straightforward and neutralizes easily, this probably represents a true ‘allergic’ reaction by the woman to her own hormones. But sometimes it can be very difficult or impossible to neutralize a symptom once provoked. We take this to be evidence that the real problem is a hormone imbalance – hormone replacement therapy (HRT) can be considered as a possibility in management.
Sublingual provocation and neutralization
A modification of the Miller-Lee technique is to test substances under the tongue (sublingually). A food or other concentrate is placed under the tongue and the reactions noted. If the patient experiences a symptom, this is neutralized, as before, by serial dilutions. The dilution that switches off the symptom completely is taken as the end-point (Dickey, LD Sublingual Use of Allergenic Extracts (monograph) ed. H C King, Elsevier, New York, 1981).
There is no essential difference between this approach and using an injection, although naturally there are fewer parameters by which to judge reactions or the lack of them. Instead of being able to view a wheal, its size and characteristic, the clinician has only the patient’s subjective symptoms to rely upon, plus what he or she can observe objectively. Yet with practice it is possible to become quite adept at spotting subtle shifts in the patient’s mood or attitude, skin colour, etc. The neutralizing dose would be that which leads the patient to declare his or her symptoms ‘switched off’ and the clinician to note that whatever manifestations arose have disappeared again.
Obviously, subtle reactions may be missed. Well-masked allergens may not react at all. But the technique is especially suitable for children, many of whom don’t like injections and would not willingly sit for several hours tolerating intracutaneous needles every 10 minutes.
Dermal application testing
A further modification of this technique, developed by Drs Jean Munro and Ray Choy in London, is to test substances directly on the skin. This method arose from an observation that probably all clinical ecologists have made form time to time: that an extremely sensitive individual sometimes feels unwell just being in the presence of allergens. Such patients may have to be relocated away from the storage and display areas there test solutions are kept in order that they can be tested.
Munro and Choy were finding that some patients were reacting quite severely to the usual technique and decided to test these patients by simply having them hold a phial of the solution. Even this was too much for some; and so dermal application was resorted to. It was found quite workable.
By placing a dilution of the extract on the skin of, say, the back of the hand, biological and subjective reactions could be provoked and then neutralized by further dermal applications. Sometimes these dilutions may reach ‘homoeopathic’ levels (i.e. they are very dilute) but still seem to work.
The important safety measure is that if a strong reaction develops, the test solution can be wiped off swiftly.
Controversy
No technique of clinical ecology has been more heavily criticized than Miller’s method. Nevertheless, most of us who use it do so because we are aware of its capabilities and accept its scientific validity. More and more papers are being published that show its effectiveness. Yet the controversy won’t go away.
Over the years a number of studies have been cited to show that Miller’s method is a fake. Almost without exception these have been improperly reported, evidence for key statements has been missing and data has been altered (or withheld) or the protocol so bad that it was obviously designed to invite failure.
In 1973 the Food Allergy Committee of the American College of Allergists, using sublingual provocation testing (see below), carried out a study that showed that the neutralization basis of Miller’s method was quite effective. Did they publish their findings? No, they repeated the whole test again in 1974 and this time found that the statistics were not as good. The second study was therefore termed ‘The Final Report’ while the first positive study was simply cast aside.
The ‘Jewett trial’ carried our in 1981-83 was appallingly defective. The results remained unpublished for seven years, so clinical ecologists world-wide were deeply shocked when it was suddenly published in August 1990 in the New England Journal of Medicine. This, the world’s second most prestigious medical journal, even went to the extraordinary length of issuing a press release announcing that at last the clinical ecologists were going to be sunk. I won’t say such spite is without precedent in medicine, but it certainly has no place in a scientific periodical.
To my mind, Miller’s method is an outstanding contribution to medicine. Like all medical techniques, it requires skill if it is to be performed correctly.
Modern SLIT (sub-lingual immunization therapy)
I mentioned that sub-lingual allergy neutralization therapy has come of age. It’s gone mainstream and appears everywhere. Yet I was called a quack (seriously) for using it in the early 1980s.
Sandra Y. Lin, MD, an associate professor of otolaryngology–head and neck surgery at Johns Hopkins University School of Medicine in Baltimore, Maryland, and colleagues did a systematic review of 63 studies with 5131 participants found moderate support for sublingual immunotherapy for the treatment of allergic rhinitis and asthma.
The findings were published their findings March 27, 2012, in JAMA.
They were not looking at food allergies, per se. They were more interested in diseases, like asthma and rhinitis. Improvements found were 40% or even more. That’s without eliminating any suspect foods, so not a bad result. I would have got closer on 85%, if allowed to enter dietary advice, as well as immunotherapy.
Still, all in all, a very satisfactory paper and much vindication of the work I and others did, back in the 1970s and 80s.
Of course the die-hards who make their money from allergy shots were quick to start picking holes.
Robert Bush, MD, professor emeritus of medicine in the Section of Allergy and Immunology at the University of Wisconsin in Madison, said:
“This paper updates the previous Cochrane meta-analysis and appears to strengthen the data regarding the efficacy and safety of [sublingual immunotherapy] by adding recent studies.”
“While the article is generally supportive of the potential use of [sublingual immunotherapy] as being efficacious and relatively safe, it is important to remember that [sublingual immunotherapy] has yet to gain FDA approval for the vaccines. Further research is needed to establish standardized dosing, and FDA approval will be necessary before [sublingual immunotherapy] is considered as a part of clinical practice.”
The sly innuendo that the FDA hasn’t approved it yet (who cares?) is to try and weaken the competition and he trots out the old chestnut “more research needed”, which is the last refuge of the intellectually dying, as they see the ground crumbling from beneath their feet!
[REFERENCE” JAMA. 2013;309:1278-1288]
Support For Miller’s Method Sublingual Therapy
I remarked in my video that sublingual immunization therapy (SLIT) has received much scientific scrutiny lately and been found very good.
I’m just publishing this note about yet another paper. It shows how disgracefully bad American science is, with them claiming the technique was first published in 1986. Just not true! It goes back decades before that.
But they ignore anything outside their own narrow purview.
Here’s a brief extract; you don’t need all the technical stuff.
Abstract
Sublingual immunotherapy (SLIT) for allergic respiratory diseases was first described in 1986 and immediately appeared as a viable alternative to the traditional subcutaneous route. Since then, more than 60 randomized controlled trials have been published, almost all with very favorable results. The average improvement over placebo in symptom score and medication use was always greater than 20%. The results of the clinical trials were pooled in several meta-analyses, which consistently confirmed the efficacy of the treatment. SLIT is characterized by a satisfactory safety profile, its side effects being mainly limited to oral discomfort. Only six anaphylaxes and no fatalities have been so far reported. Due to the good risk: benefit ratio, SLIT is currently being investigated in diseases other than respiratory allergy, such as food allergy and atopic dermatitis.
[Immunotherapy. 2013;5(3):257-264]
Introduction
In 1986 the use of allergen-specific immunotherapy (SIT) administered by the sublingual route (SLIT) was described for the first time. Until then, the only route of administration for SIT remained subcutaneously (SCIT), which was repeatedly demonstrated to be effective in respiratory allergy. Nonetheless, with SCIT, some risk of severe or even fatal adverse events still remains.
The risks can be partly attributed to technical/human errors and can therefore be avoided; however, a large fraction of the severe adverse events reported remain unpredictable, even if all precautions are taken. Based on this, alternative routes of administration were repeatedly approached. Among them, SLIT appeared as a promising route, despite initial skepticism owing to the low doses used and the poor design of the early studies. During the last 15 years, numerous randomized controlled trials confirmed the clinical efficacy of this route and several surveys supported the good safety profile of SLIT. Nowadays, SLIT is officially accepted in international documents as a viable alternative to SCIT for both adults and children. In addition, thanks to the good safety profile, the use of SLIT has also recently been proposed in non-respiratory allergy, including atopic dermatitis and food allergy.
[please note I was using it for food allergy as early as 1981! My mentors go back before that even. Carleton Lee discovered the neutralizing method as long ago as the 1950s. It has been proposed that it be called the Lee-Miller Method]
Despite the abundant literature confirming the efficacy of SLIT, some aspects are still debated, such as the optimal maintenance dose, best administration regimen and duration of the treatment. Finally, the wide variability in standardization methods, usually applied using in-house references, render the published studies difficult to compare.
Cytotoxic Tests
This next method sounds closer to the classic antibody blood tests, such as the ELISA. However there are significant differences and it is far from mainstream yet.
Use of a ‘leucocyto-toxic’ reaction for in vitro screening for food allergy antibodies was first recorded by P. Black in 1956. The test at that time was crude and produced results that are best described as suggestive, rather than conclusive. Today’s method follows 30 years of refining this test.
Since 1960 the test has been researched steadily by W.T.K. Bryan and M.P. Bryan at Washington University school of Medicine in St Louis, Missouri. The technique is simple but depends for accuracy upon a high standard of laboratory technique.
White blood cells (leucocytes), separated by centrifuging, are placed on a microscope slide chamber and mixed with about 10 mg of food extract. The sample is then observed at intervals over the next two hours, using a x 60 lens, and the effect of the food extract on the white cells is noted.
Healthy white cells are mobile and exhibit amoeba-like behaviour. On contact with an allergen, in this case a food sample, the cells lose their mobility and become rounded in shape. Cytoplasmic granules become sluggish and cease to stream. Eventually, damaged cells rupture and die. Hence the name for this procedure which is cyto (cell).. toxic (damaging).
A typical test might include several dozen foods, food additives and inhalants such as dust, cigarette smoke and even house gas. Theoretically, hundreds of items at a time can be tested. In practice, the number of items is limited by how many technicians are employed and how many slides they can scrutinize before the samples begin to deteriorate.
Reporting
It is customary to grade reactions from 0 to 4, depending on severity of damage, observing the following changes:
0 reduction or loss of amoeboid movement
0 reduction or loss of amoeboid movement
1 intracellular stasis (slow-down or stop-page)
2 rounding and distortion of cell contour
3 vacuolation (the appearance of tiny vacuoles, or cavities)
4 cell lysis (bursting open)
Dr. Damien Downing, who first introduced this method into the UK, claims that it has an 80 per cent accuracy. There are many critics however, even among clinical ecologists, who do not take these claims seriously and who point to many well-conducted trials which show that the method is virtually useless. Cytotoxic testing appeared to suffer a mortal blow to its credibility when, for a stunt, journalists sent blood from the same person on the same day and received two widely different reports on the “patient’s” sensitivities.
The difficulty with the test, in common with many other methods, is that it rests in the final analysis on human interpretation rather than objective measurement. This isn’t so bad as long as each laboratory is at least consistent with its own standards. But it may, on occasion, lead to patchy quality in results, which can be very misleading for the patient.
Dr Downing comments on the reproducibility of the test: ‘If the same blood is examined in two separate preparations simultaneously, or in the same preparation by two technicians, or the same blood is examined at 24-hour intervals under controlled conditions, with any single increase in the degrees of freedom, one generally finds that between one in five and one in six of the test results cross the border form one to another of the four possible results. This is presumably a reflection of the technicians’ human limitations. Greater degrees of variability are rare, at around one per cent. That is to say that a technician can manage to, get the result accurate to within one degree of reaction 99 per cent of the time!’
This sounds almost too good to be true, until you remember that in this case each ‘one degree’ of reaction represents 20 per cent of the whole; that means results could be in error by 39% of effect and yet still appear as only “one degree” apart!
Modern test systems, such as the ALCAT or Nutron test claim to get round this element of observer error by using mechanized counting.
Probably the main drawback of the cytotoxic test method is that it needs intelligent and knowledgeable back-up by a competent doctor. Otherwise the patient is left avoiding certain foods indefinitely, with no clear place in mind, struggling to keep up an adequate diet n a selection of things to eat that may be pitifully limited.
Unfortunately, this after-care is not always readily obtainable and the laboratories themselves often duck the issue.
Leave a Reply
You must be logged in to post a comment.